Many infectious diseases generally have different seasonal patterns; the flu has a peak in winter, chickenpox in spring and hepatitis A in summer1. Many viral respiratory diseases have a so-called seasonality or the oscillation in the available number of actual pathogens which determines the contagiousness of the disease during the year.
But what determines seasonality and what can be said about the current COVID-19 pandemic?
Unfortunately, the mechanisms that determine seasonality remain poorly understood. But in general some theories have tried to explain this phenomenon in terms of several concomitant effects:
- The different ability of the immune defenses to fight disease as a consequence of climatic conditions;
- The different weather conditions such as temperatures and humidity which could determine whether the virus will survive outside for a sufficient time for the infection;
- The behavioral and contact habits of people that determine the transmission of the virus (for example, spending more time indoors in close proximity to other people such as in schools or ski resorts).
Predicting which of these coexisting effects can determine the seasonality of a new epidemic such as COVID-19 is complex. Some speculate that it may even have no seasonality and become endemic in the future. For now, all containment strategies are based on the concept of limiting transmission by means of social distancing in order to make the national health service able to deal without problems with the number of patients suffering from major respiratory problems.
However, once it has been established that a viral disease has a certain confirmed seasonality, as for example in the flu, it is possible to deploy vaccination policies (where available) with a precise timing that can follow the virus sub-type (for example A / H1N1) and as the winter season approaches, vaccinate those most at risk. This "flu season" calendar is very similar for countries with similar latitude and inverted for countries north or south of the equator; in general we prepare for the new wave of contagions following the approach of the cold seasons with low humidity.
In principle, given the knowledge and model of virus propagation for one hemisphere of the earth, a possible forecast could be made for what will be the spread in the countries of the other hemisphere.
COVID-19 has mostly affected the northern hemisphere with China, Iran, Europe and North America during the winter months (April 9, 2020) but has also affected some countries south of the equator such as New Zealand, Australia and marginally some Pacific islands such as Guam, French Polynesia with tropical climate currently hot and humid (conditions seem unfavorable for COVID-19).
This could suggest that the virus does not have a dependence on air temperature and humidity, as in the case of influenza, leading to the non-seasonality of COVID-19. In any case, the lack of immunity of the population to the new virus adds a variable to the complexity of the model which makes the data difficult to read and the forecasts unreliable. What effect is dominant in this case? Difficult to know.
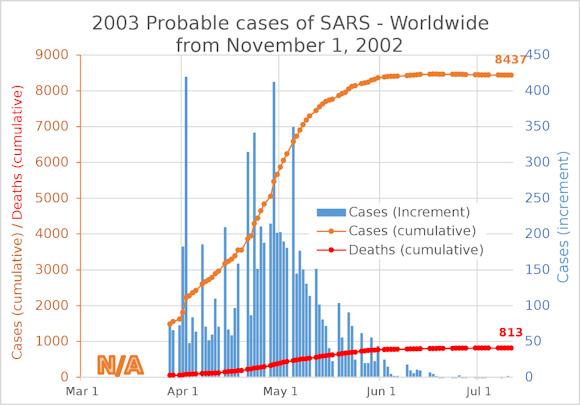
Current COVID-19 is part of a family of seven types of Coronaviruses that infect humans, including SARS-CoV and MERS-CoV which can cause acute respiratory problems. The 2003 SARS coronavirus outbreak (virus that has many structural similarities to the current virus) infected the first human in Guangdong province in China has been followed and accurately recorded by the World Health Organization and therefore perhaps it is possible draw some lessons from its numbers. In this case the epidemic caused about 8000 cases and had a relatively short duration but no conclusion can be drawn on the possible seasonality. This is because it was quickly contained as the summer months approached. Who or what caused the end of the infection is not clear: perhaps the improvement of sanitation conditions, perhaps the approach of summer.
The Middle East respiratory syndrome-related coronavirus (MERS) coronavirus epidemic has infected approximately 2012 patients with an extremely high mortality of 2500% since 34. The first case of this pathology was recorded in Saudi Arabia and, considered the widest time window, it could provide additional indications on the seasonality of a component of the coronavirus family. A publication from the University of Health Sciences, Riyadh, Saudi Arabia2 analyzed the data and came to the conclusion that the epidemic is following a clearly declining trend which suggests that, if nothing changes, the disease could disappear in the near future. The publication also analyzed the seasonality of MERS and found a 14% decrease in the number of cases in certain months of the year, in short, statistically insufficient to confirm the seasonality thesis.
However, a study that argues in favor of the possible seasonality of SARS Coronavirus is that presented by KH Chan in 20113 in Advance in Virology, according to which this virus is much more stable and effective at low temperatures and low humidity characteristic of the winter months. By surviving the virus longer in the air and on surfaces, the ability to transmit to other individuals is increased. It remains to be seen, of course, whether COVID-19 also has similar characteristics, although preliminary studies support this hypothesis. The importance of temperature and humidity conditions is also confirmed by a study from the University of Maryland4 which showed that COVID-19 spread more easily in countries and regions of the world whose temperatures were between 5 and 11 ° C and low relative humidity.
At present, we have data and models that give conflicting information and no conclusion on the possible seasonality of COVID-19 is possible. This conclusion is also confirmed by a recent report compiled by experts from the National Academies of Sciences, Enginering and Medicine5. We cannot rely on numerical transmission patterns of the virus that nobody has tested yet.
The numbers so far show that social distancing works and remains one of the few weapons available right now to reduce the rate of growth of the pandemic. The combined effect of temperature, humidity, UV exposure on the stability of the virus, however, keeps alive the possibility that there may be a partial attenuation of contagiousness in the summer months and gives governments time to prepare for the next wave of contagions likely in the future winter months. .
Image Number of SARS cases (2002-2003): Cumulative cases in orange, daily increments in blue and cumulative number of deaths in red.
1 Martinez, The calendar of epidemics: Seasonal cycles of infectious diseases. PLOS Pathogens (2018)
2 Ahmed et al, Underlying trend, seasonality, prediction, forecasting and the contribution of risk factors: an analysis of globally reported cases of Middle East Respiratory Syndrome Coronavirus. Epidemiol Infect (2018)
3 KH Chan et al, The Effects of Temperature and Relative Humidity on the Viability of the SARS Coronavirus. Advances in Virology (2011)
4 Sajadi et al, Temperature, Humidity and Latitude Analysis to Predict Potential Spread and Seasonality for COVID-19. SSRN (2020)
5 Rapid Expert Consultation on SARS-CoV-2 Survival in Relation to Temperature and Humidity and Potential for Seasonality for the COVID-19 Pandemic. National Academies of Sciences, Engineering, and Medicine (April 7, 2020)